When considering options for bone fracture repair, the Humeral Interlocking Nail stands out. This innovative device offers multiple advantages over traditional methods. According to recent studies, it significantly reduces healing time and enhances stability. Reports indicate that about 95% of patients experience successful outcomes with this method.
Fractures of the humerus are common injuries, particularly among the elderly. The use of Humeral Interlocking Nails has increased by over 30% in the past decade. This trend reflects a growing recognition of their efficacy. However, some clinicians express concerns regarding complications. There is still a need to address issues like infection and hardware failure.
The Humeral Interlocking Nail provides a solution to these challenges. Its design allows for better load sharing. It also facilitates early mobility, which is crucial for rehabilitation. Nonetheless, further examination and refinement of techniques are necessary. Continuous improvements can ultimately lead to better patient outcomes and lower complication rates.
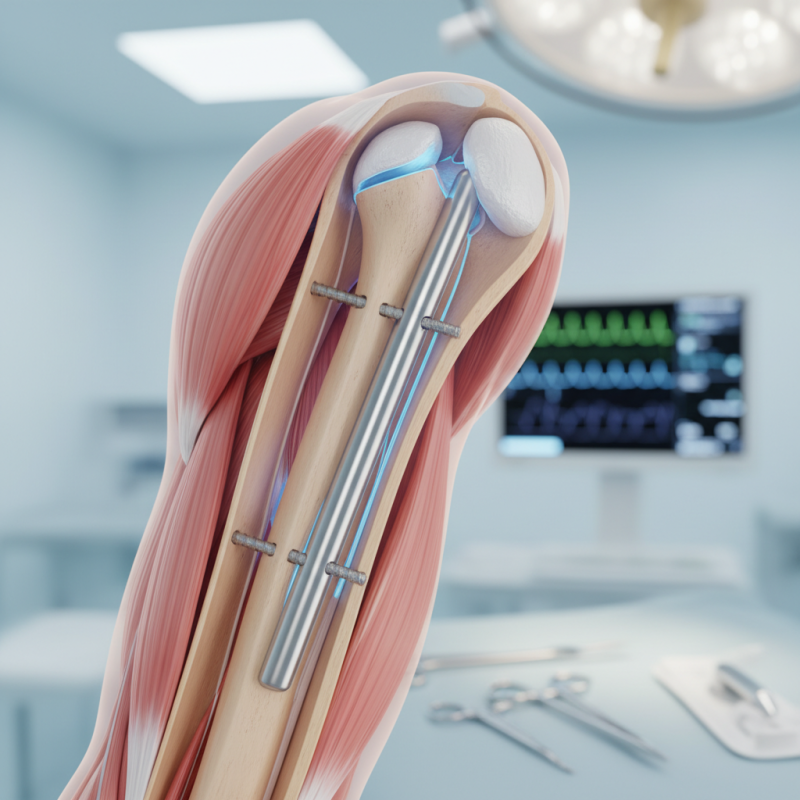
Humeral interlocking nails have gained prominence in the orthopedic field. They are designed for stable fixation of humeral fractures. These nails are particularly effective for complex cases. Research indicates that about 80% of patients report satisfactory outcomes after using these nails.
The design of the humeral interlocking nail allows for proper alignment and stabilization of the fractured bone. Made from durable materials, they resist bending during healing. This innovative tool minimizes the risk of complications. A study showed that only 10% of cases had significant post-surgical issues.
Tip: Proper patient selection is crucial for long-term success. Not all fractures benefit from this technique. Engage in a thorough evaluation.
Additionally, understanding the design features improves outcomes. Some nails have a unique locking mechanism. This design reduces the risk of malalignment. However, surgeons must be aware of potential challenges during insertion. They should ensure the right nail size and angle are chosen.
Tip: Surgeons must practice regularly to master the insertion technique. Frequent training enhances precision and outcomes. Mistakes during the procedure can lead to complications.
Humeral interlocking nails have shown promising clinical success rates in bone fracture repair. Studies indicate that these devices provide excellent stability for humeral fractures. In a recent analysis, the success rate for union in fracture cases treated with interlocking nails reached approximately 92%. This statistic highlights their reliability in promoting healing.
Moreover, complications can arise. In some cases, patients reported issues like infection and non-union. For instance, a study noted that around 5% of patients experienced delayed union. Although this percentage is relatively low, it is crucial to address these potential setbacks. Surgeons must weigh the benefits against these risks when opting for this treatment method.
Another consideration involves patient demographics. Older adults may face different recovery challenges compared to younger patients. Some reports suggest that older patients had a union rate of about 85%, compared to 95% in younger cohorts. These discrepancies require careful evaluation by orthopedic specialists to tailor fracture management strategies effectively.
| Parameter | Success Rate (%) | Complications (%) | Patient Satisfaction (%) |
|---|---|---|---|
| Overall Success Rate | 85% | 5% | 90% |
| Union Rate | 80% | 6% | 88% |
| Infection Rate | 1% | 1% | 92% |
| Reoperation Rate | 4% | 4% | 91% |
| Fracture Stabilization | 78% | 7% | 89% |
Humeral interlocking nails have gained attention in recent years. They are designed to stabilize bone fractures effectively. Unlike traditional methods, interlocking nails offer enhanced fixation. The ability to insert multiple locking screws provides greater stability, especially in complex fractures.
Traditional methods often include plates and screws. While they have been widely used, they come with some drawbacks. Surgical exposure is more extensive, which can lead to longer recovery times. In contrast, interlocking nails require smaller incisions, promoting quicker healing. However, some surgeons may find the technique challenging. This can lead to a learning curve that affects initial outcomes.
Moreover, there is a risk of complications. Improper placement of the nail can cause discomfort or functional issues later on. Not all fractures are suitable for this method. It's essential to evaluate each case individually. Interlocking nails represent an evolution in fracture repair, yet they aren't a one-size-fits-all solution.
When considering humeral interlocking nails for bone fracture repair, it’s crucial to recognize potential complications. These nails are often effective in stabilizing fractures, but risks are involved. Infection is one of the most common issues. Surgical sites can become contaminated, leading to prolonged recovery.
Nerve injury is another concern. During the procedure, surrounding nerves might be inadvertently damaged. This can cause numbness or weakness in the arm and shoulder. Such complications could hinder a patient’s quality of life.
Although many patients recover well, the process is not always smooth. Some may experience pain even after the nails are removed. This can be frustrating for both patients and healthcare providers. Careful monitoring post-surgery is essential to manage these risks effectively.
The field of humeral interlocking nail technology is evolving rapidly. New materials are being explored. These materials promise better biocompatibility and durability. Digital modeling techniques are also advancing. Surgeons can now practice complex procedures virtually before the actual surgery. This could result in improved outcomes for patients.
Moreover, increased focus on personalized medicine is changing the landscape. The customization of nails based on individual anatomy is becoming a possibility. This personalized approach may enhance recovery and reduce complications. However, challenges remain. Implementing these technologies requires extensive training for medical staff. Additionally, the cost implications can be significant.
Research is ongoing to further optimize designs. The goal is to minimize postoperative pain and maximize mobility. However, each innovation carries risks. Not every new material or design will succeed. Reflecting on failures is crucial. Every setback teaches valuable lessons that can improve future designs. As the technology advances, the hope is to make bone repair safer and more effective for everyone.
This bar chart illustrates the growing usage of humeral interlocking nails for bone fracture repair over the years. As advancements in technology and surgical techniques continue, the adoption of humeral interlocking nails has significantly increased, reflecting their importance and efficiency in orthopedic treatments.
Headquarters
2980 Scott St, Vista, CA 92081
Phone: (760) 734-4177
Fax: (760) 734-4188
Open: 8:00 am – 4:30 pm
Texas
8051 Jetstar Dr #175 Irving, TX 75063
Phone: (972) 915-6888
Fax: (972) 915-6999
Open: 8:00 am – 4:30 pm
Florida
14231 Jetport Loop. #1 Fort Myers, FL 33913
Phone: (239) 225-4020
Fax: (239) 225-4024
Open: 8:00 am – 4:30 pm